Criterion 2.3-11: Ensuring the safety of newborns at birth: a quality imperative
Criterion 2.3-11 is a key pillar for ensuring the safety and well-being of newborns from the very first moments of their lives. It outlines the requirements for healthcare teams to provide optimal and continuous care, with the goal of improving the infant’s health and quality of life.
What is Criterion 2.3-11, and why is it essential?
Criterion 2.3-11 is a key indicator for maternity units and is considered essential.
Its main objective is to ensure the safety of newborn care at birth, which is directly linked to improving the newborn’s health and well-being from the very first moments. This involves a series of standardized and systematic actions that healthcare teams must follow.
This criterion covers several key aspects of initial newborn care, including:
- Immediate identification of the infant.
- Prevention of infections.
- Assessment of vital signs, often using the Apgar score.
In essence, it aims to organize practices so that every newborn benefits from a safe environment and appropriate care from birth, anticipating needs and potential risks.
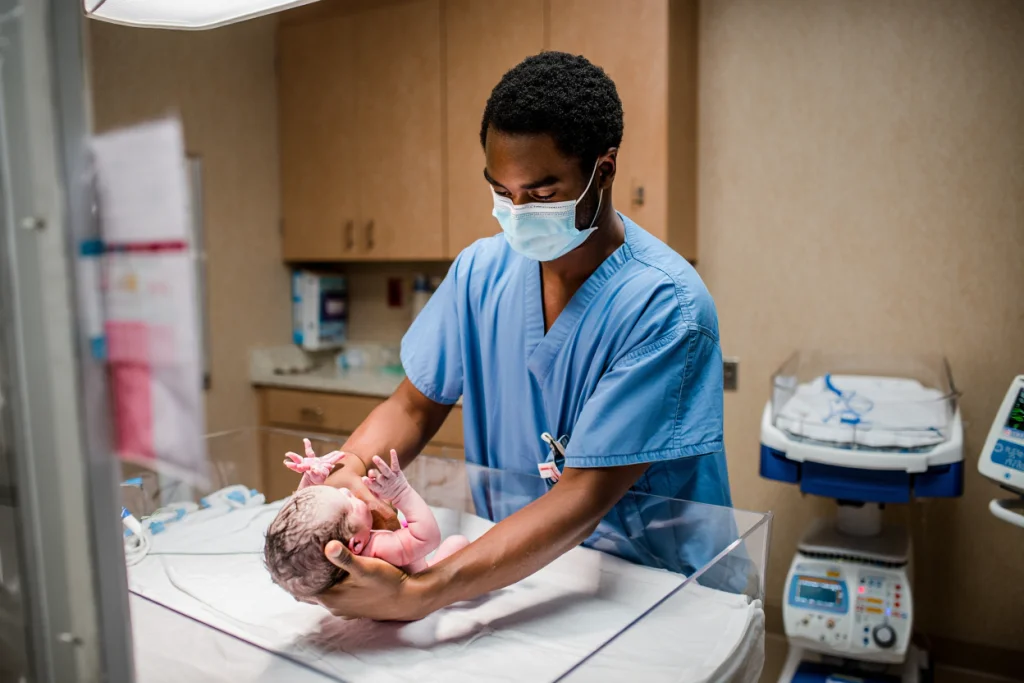
The foundations of security: Continuous care and monitoring
To meet the objectives of Criterion 2.3-11, particular attention is paid to continuous monitoring and the provision of essential care. Continuous monitoring enables the rapid detection of any abnormality or complication that would require specialized care.
Essential care routinely provided includes:
- Maintaining body temperature. This is all the more crucial given that the neonatal resuscitation protocol emphasizes temperature maintenance, particularly for premature infants, for whom drying, swaddling, and the use of a plastic bag are key measures. Healthcare professionals must also take the newborn’s temperature upon discharge from the delivery unit and upon admission to the intensive care unit.
- Managing feeding, including support for breastfeeding, which must be part of a formalized quality assurance process.
Furthermore, clear communication with parents is essential to ensuring a smooth transition and promoting close monitoring of the newborn’s first moments of life. Specific actions such as delayed umbilical cord clamping and skin-to-skin contact are practices that healthcare professionals must document, explaining the reasons if they are not performed. These measures contribute to better adaptation to extrauterine life, which, in the majority of cases (85%), occurs naturally, but sometimes requires stimulation or, for 5% of infants, positive pressure ventilation. The pivotal role of healthcare professionals: Training and quality improvement. The success of Criterion 2.3-11 largely depends on the skills and commitment of healthcare professionals. It is imperative that all professionals caring for newborns in the delivery and maternity ward receive simulation-based training from the start of their employment and throughout their professional practice. This training includes mastering care procedures, particularly regarding neonatal resuscitation and the management of neonatal infections. Newborn resuscitation is primarily respiratory, with only one in 1,000 newborns requiring chest compressions. To facilitate this adaptation, anticipating preparation, checking equipment, ensuring the availability of caregivers, and using checklists are essential to minimize stress and ensure readiness. Managing an emergency situation is a true team effort, requiring a clearly identified leader, good coordination of actions, and information sharing.
In addition, professionals are required to:
- Document the delayed cord clamping, skin-to-skin contact, and the newborn's temperature in the patient's medical record.
- Participate in a formalized quality improvement process, such as one focused on breastfeeding support.
- Analyze their results and identify measures for continuous improvement, such as those related to the rate of delayed cord clamping, antenatal corticosteroid therapy, or length of hospital stay.
This approach ensures continuous improvement in practices and optimal safety in the care provided to newborns.

Safeteam's P25 training: A concrete measure for Criterion 2.3-11
The "Strengthening Your Practices in Case of Neonatal Resuscitation (P25)" training offered by Safeteam is directly aligned with the requirements of Criterion 2.3-11, particularly the requirement for professional training. This training is intended for a diverse audience, including childcare assistants, nurses, midwives, anesthesiologists/intensivists, and pediatricians working in the delivery room.
The main objective of the P25 training is to enable participants to manage a newborn in cardiac arrest in accordance with the current international guidelines of the European Resuscitation Council (ERC). This is crucial because neonatal resuscitation is a skill that professionals must master under Criterion 2.3-11.
The training focuses on:
- Mastering best practices in resuscitation, such as the ABCDE algorithm (Airway, Breathing, Circulation, Drugs, Environment). This algorithm includes airway management, positive pressure ventilation (PPV), chest compressions, increasing FiO2, and tracheal intubation if necessary. Upper airway suctioning is also part of the clearance process and should be performed with caution, never routinely. Securing and ensuring reliable communication protocols, including alerts and handovers. Reducing the risks associated with iatrogenic hypothermia. The teaching methodology is innovative, combining independent learning with group sessions via videoconference. It uses immersive video simulation to recreate the care provided to a newborn in cardiac arrest by a multidisciplinary team, followed by a video debriefing with field experts. This approach raises awareness of the importance of human factors and teamwork in emergency situations, providing concrete tools for immediate implementation. By regularly practicing as a team and using cognitive crisis management aids, professionals can significantly improve the quality of care, even under stress or fatigue.




