Non-invasive ventilation (NIV) is an essential method for treating respiratory failure, whether acute or chronic. Unlike invasive ventilation, which requires an endotracheal tube or tracheostomy cannula, NIV uses a face or nasal mask to deliver positive pressure without directly entering the airways. This method improves gas exchange by reducing carbon dioxide in the blood and increasing oxygenation. It also decreases respiratory effort while avoiding the complications associated with invasive intubation. Used for conditions such as sleep apnea syndrome, COPD, or obesity hypoventilation syndrome, NIV is an effective alternative in intensive care or at home. However, its success depends on rigorous monitoring to guarantee its effectiveness and tolerability. This technique represents a major advance, offering tailored and less restrictive care.
What is NIV?
Non-invasive ventilation (NIV) is a method of mechanical ventilation that does not require the use of an invasive artificial airway, such as intubation or tracheostomy. It works by delivering positive pressure through a tight-fitting mask covering the nose, or the nose and mouth. This allows the patient to breathe spontaneously while receiving appropriate ventilatory support.
This technique ensures satisfactory alveolar ventilation by improving gas exchange and reducing the concentration of carbon dioxide in the blood. Unlike invasive ventilation, NIV reduces the risk of complications, such as infections and airway injuries, often associated with intubation. Several types of masks are used in NIV, ranging from nasal masks, which are often better tolerated because they are less bulky, to oronasal or full-face masks, which offer a better seal. This system allows for the application of positive pressures adjusted according to the patient's specific respiratory needs. NIV differs from invasive ventilation, which requires an endotracheal tube or a tracheostomy tube inserted directly into the upper airway. This latter option is reserved for patients with severe respiratory failure or in emergency situations where NIV would not be effective. Developed from the 1980s onwards, non-invasive ventilation experienced strong growth in the 2000s, particularly for treating obstructive respiratory disorders, decompensated COPD, and certain forms of chronic or acute respiratory failure. Today, it is a major component of respiratory therapy, used in hospitals, intensive care units, and even at home.
The different modes of NIV

Non-invasive ventilation (NIV) is a technique that can be adapted to the specific needs of each patient patient, depending on the nature and severity of their respiratory distress. The main modes of NIV are distinguished by how the ventilator controls the volume of air delivered and the pressure applied during the respiratory cycle.
The main types are:
1. Pressure Support Ventilation (PSV): This mode assists the patient's spontaneous breathing by providing positive pressure during inspiration, which facilitates the work of breathing without imposing a fixed volume. In addition, positive end-expiratory pressure (PEEP or PEPAP) helps maintain open airways during expiration.
2. Pressure-controlled ventilation: In this mode, the ventilator applies a fixed pressure for a set duration, generating a variable air volume based on lung compliance and airway resistance. This mode is particularly used in cases of acute respiratory failure, when the patient is less independent. 3. Volume-controlled ventilation: Here, the ventilator delivers a constant air volume with each breath. The pressure then varies according to the patient's lung characteristics. This mode is less common in NIV, however, because it can cause discomfort if the pressure is not sufficiently adjusted. 4. Mixed or programmable modes: Modern devices allow for combining pressure and volume or alternating assisted and controlled phases (for example, in "assisted-controlled" mode). These modes offer great flexibility for optimizing respiratory care. Ventilators used in NIV are often equipped with humidifiers to warm and humidify the delivered air. This improves patient comfort and limits dryness of the upper airways. These devices can be portable, making them suitable for use in both intensive care and at home. The choice of ventilation mode depends on several factors: clinical indications, the pathological context, but also the patient's tolerance and their interaction with the mask and equipment. A thorough understanding of the different NIV modes allows for personalized and effective treatment, minimizing discomfort while maximizing the chances of success for non-invasive ventilation.
Clinical indications for NIV
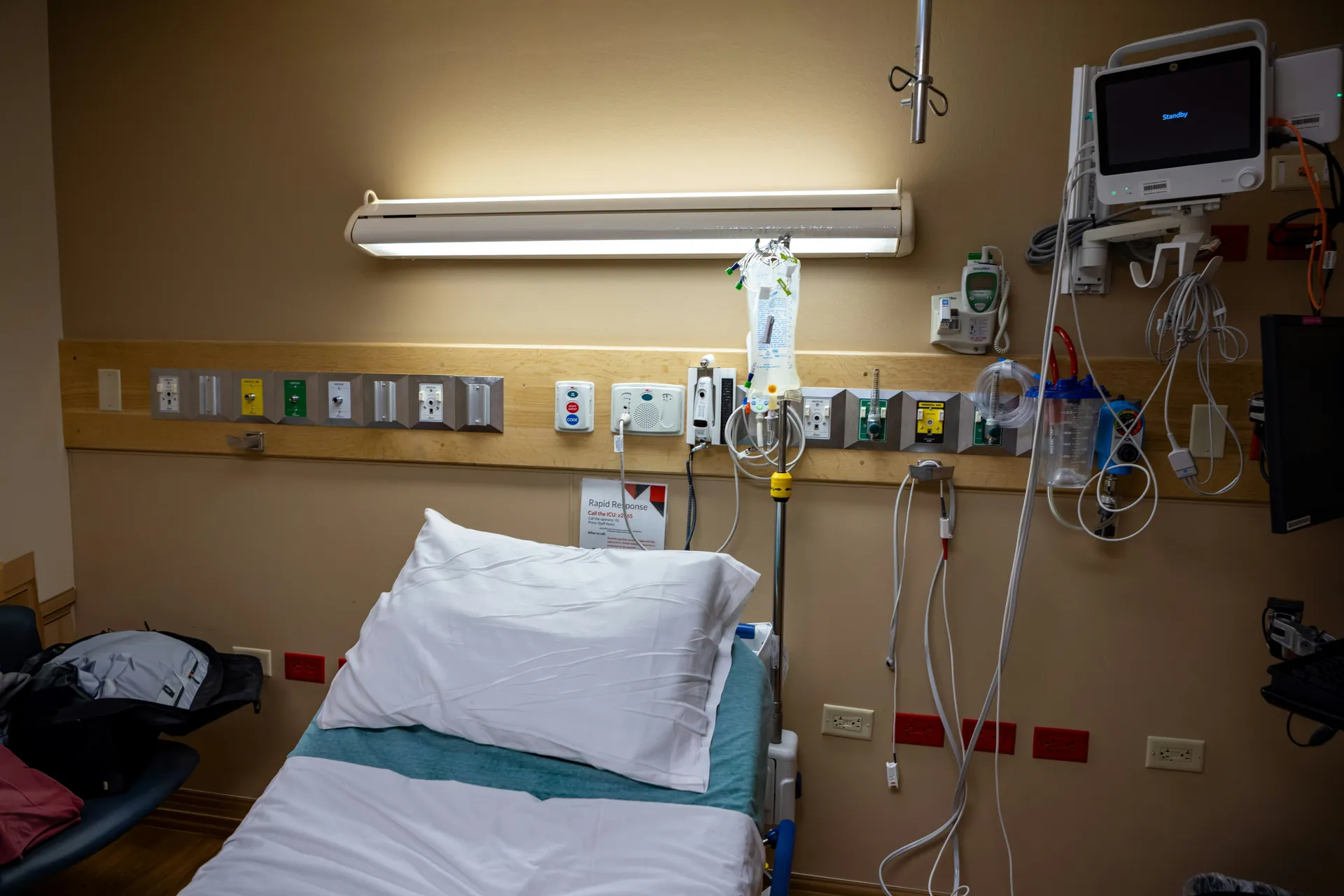
Non-invasive ventilation
Invasive ventilation (NIV) is primarily used to treat respiratory failure, whether acute or chronic. It is indicated when the patient has difficulty maintaining effective ventilation without resorting to invasive intubation. This method is particularly recommended in cases of acute exacerbations of chronic respiratory diseases, such as chronic obstructive pulmonary disease (COPD). It helps reduce hypercapnia, improve ventilation, and decrease respiratory workload. Furthermore, NIV plays a crucial role in the management of sleep apnea syndrome. It helps maintain upper airway patency through continuous positive airway pressure (CPAP) ventilation. This procedure prevents upper airway collapse during sleep, while improving sleep quality and oxygenation. In situations of acute respiratory failure, non-invasive ventilation (NIV) is frequently used in intensive care to avoid intubation, particularly in the presence of hypercapnia associated with respiratory acidosis. This approach helps reduce infectious morbidity and complications related to invasive ventilation, while increasing the chances of survival and decreasing the length of stay in intensive care. Furthermore, NIV may be indicated in other situations, such as the prevention of post-extubation respiratory failure, weaning from mechanical ventilation in chronic patients, or the management of respiratory disorders in immunocompromised patients. In these cases, its implementation must be carried out with caution and under close monitoring to ensure its effectiveness and avoid severe respiratory failure. Finally, NIV can also be prescribed as a home mechanical ventilation treatment for patients with chronic respiratory failure. This approach helps improve their quality of life and better control the disease outside of a hospital setting. Advantages and limitations of NIV. Non-invasive ventilation (NIV) offers many advantages, including increased comfort for the patient due to the absence of intubation and its less invasive nature. By using a mask for ventilation, it avoids common complications associated with invasive ventilation, such as nosocomial infections related to the endotracheal cannula or airway injuries. Furthermore, this technique reduces respiratory effort by providing positive pressure support, which helps improve the quality of life for patients, particularly those with chronic obstructive pulmonary disease (COPD) or obesity hypoventilation syndrome. Another major advantage of NIV is its ability to reduce hospital stays and limit prolonged use of intensive care. This translates into optimized hospital resources and lower resuscitation costs. Furthermore, NIV facilitates the implementation of home mechanical ventilation, thus offering patients greater autonomy while ensuring effective treatment of chronic respiratory failure. However, NIV has certain limitations. It is not suitable for patients with significantly altered levels of consciousness, severe upper airway obstruction, or extreme respiratory failure requiring rapid invasive intervention. The effectiveness of NIV also depends on mask tolerance. Some individuals may experience discomfort, air leaks, or develop skin irritation due to prolonged contact with the equipment. Close monitoring therefore remains essential to detect any failures of NIV, which could lead to more serious respiratory decompensation if invasive treatment is delayed. In summary, NIV represents a compromise between effectiveness and invasiveness. It offers suitable respiratory support for many patients while limiting the risks and constraints associated with invasive ventilation treatments.
Implementation of NIV
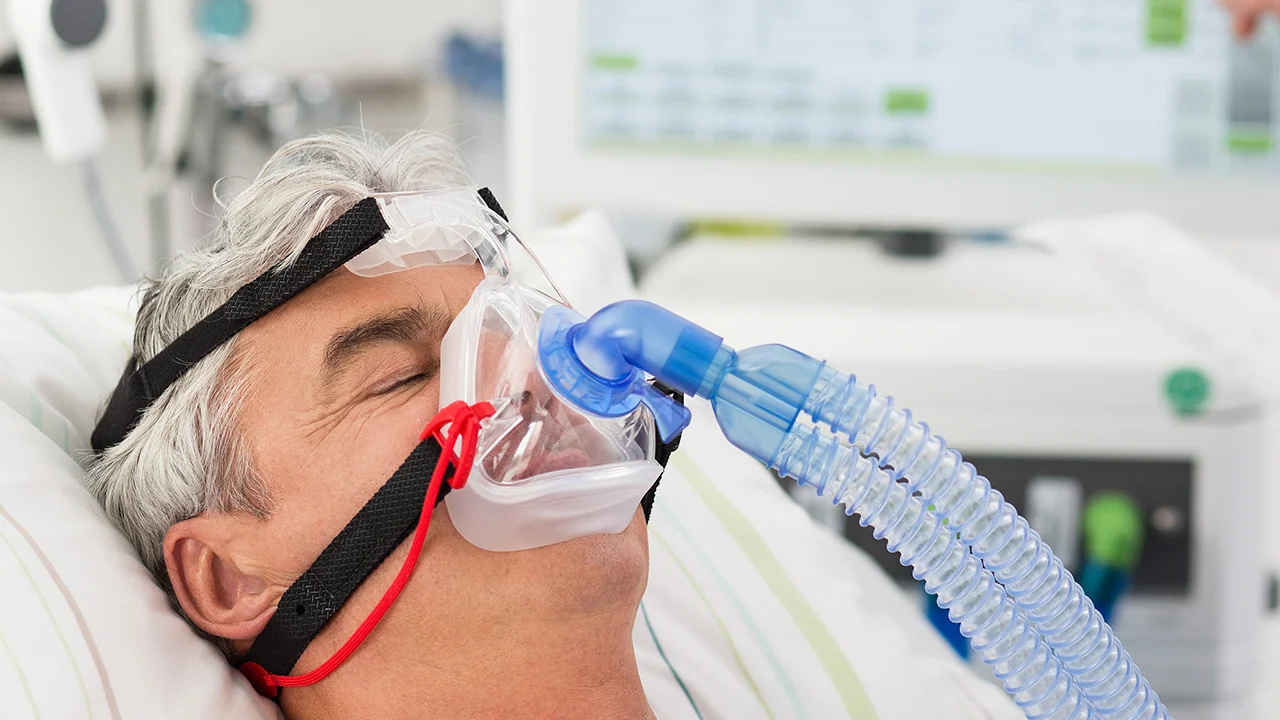
Success and discontinuation criteria of NIV
The implementation of non-invasive ventilation (NIV) requires a gradual and personalized approach. It all begins with a rigorous selection of the most suitable mask and ventilator settings, defined by the physician. Trials are then conducted in a hospital setting, generally in a pulmonology or intensive care unit, to assess the patient's tolerance and the effectiveness of the treatment on their respiratory function.
These preliminary trials allow for the prescription of a device that can be used at home, with appropriate monitoring. Patient training on the equipment is essential, as is informing their family and friends. This promotes better adherence to treatment and smoother daily management of NIV.
The success of NIV relies on several key elements: an optimal seal of the mask, good synchronization between the machine and the patient, and precise adjustment of ventilatory parameters. These adjustments aim to achieve measurable results, such as a decrease in blood carbon dioxide pressure and improved oxygenation. A gradual adaptation, often spread over several nights, is essential to optimize both patient comfort and adherence to treatment.
The criteria for stopping NIV are defined by clinical signs of significant improvement: progressive normalization of blood gases, reduction in the work of breathing, and hemodynamic stability. However, if the situation deteriorates, if respiratory failure worsens, or if the patient does not tolerate ventilation despite adjustments, invasive ventilation in intensive care may become necessary. In summary, the implementation of NIV relies on careful monitoring, personalized technical adjustments, and close collaboration between the patient and the medical and paramedical team. The goal is to ensure maximum effectiveness while minimizing the risks and constraints associated with treatment. The role of the healthcare team in the success of NIV: The healthcare team plays a fundamental role in the success of non-invasive ventilation (NIV). Their involvement contributes not only to the proper initiation of ventilation, but also to its monitoring and the patient's daily support. The effectiveness of NIV relies heavily on effective coordination between physicians, nurses, physiotherapists, and other healthcare professionals. Physicians, specialists in pulmonology or intensive care, are responsible for determining the need for NIV, choosing the appropriate interface type, and adjusting the ventilation parameters. Their expertise is essential for assessing clinical and biological responses and adjusting treatment accordingly. Nurses provide continuous patient monitoring, checking mask comfort and ventilation tolerance. They also play a key role in educating patients on the use of NIV, providing advice and support, particularly during sessions in the hospital or at home. Their regular presence facilitates a gradual adaptation for the patient and allows for the rapid detection of any complications or signs of respiratory failure. Respiratory physiotherapists intervene to maintain lung function, particularly by helping to manage bronchial congestion. They also teach assisted coughing techniques, which are essential for optimizing the effectiveness of non-invasive ventilation, especially in patients with muscle weakness or chronic respiratory conditions. Furthermore, the healthcare team coordinates overall medical follow-up, including monitoring blood gases and respiratory parameters. It also establishes a link with the maintenance services for equipment and the management of products related to mechanical ventilation, thus ensuring comprehensive and effective care. This multidisciplinary collaboration makes it possible to offer individualized support, taking into account the physical, psychological and social needs of the patient. This is crucial for the long-term success of NIV, whether in a hospital setting or with home mechanical ventilation.
Impact of NIV on clinical course
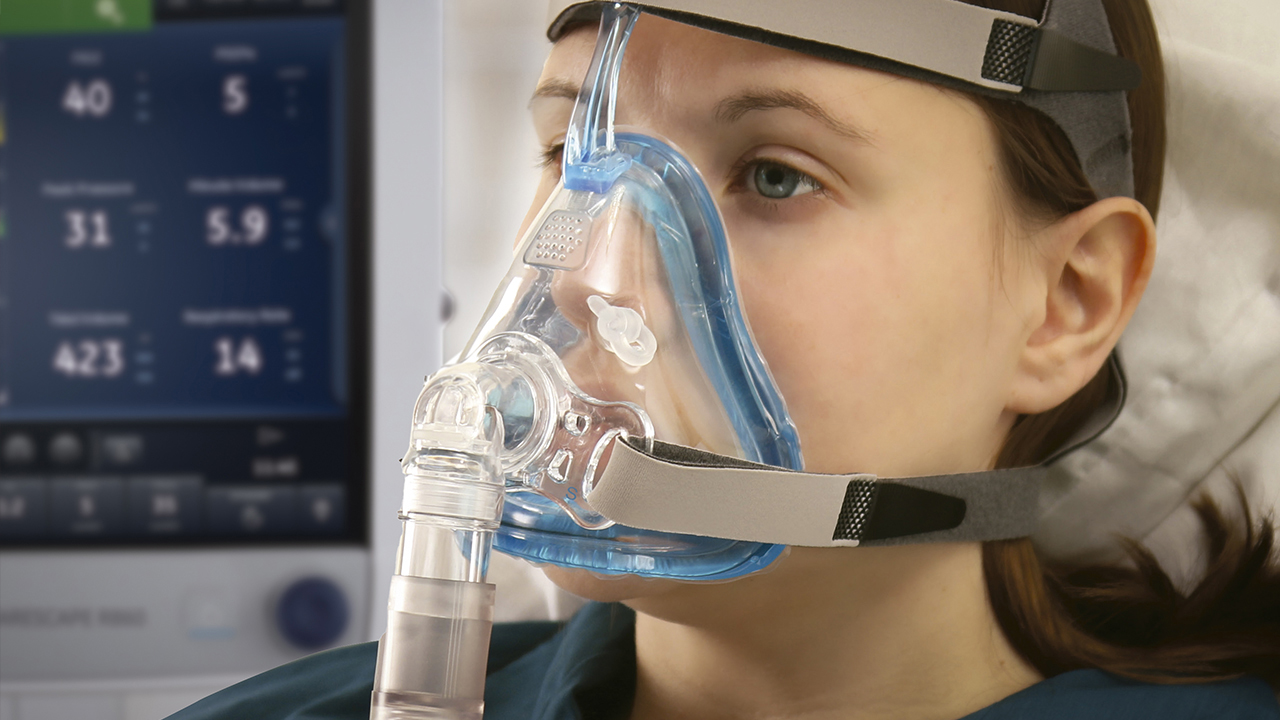
Conclusion
Non-invasive ventilation (NIV) represents a major advance in the treatment of respiratory failure. It offers effective support while preserving patient autonomy. Easily adaptable to different settings, this method reduces the need for invasive ventilation and its complications, while improving quality of life. In some cases, it even makes home care possible.
The success of NIV relies on good patient selection, rigorous implementation, and attentive support from a dedicated healthcare team. Don't hesitate to consult your doctor to determine if NIV is suitable for your situation.
FAQ
What is non-invasive ventilation (NIV) and how does it work?
Non-invasive ventilation (NIV) is a method of mechanical respiratory support that delivers pressurized air through a face, nasal, or oronasal mask, without the need for intubation.
This technique helps to maintain open airways and improve alveolar ventilation in patients with respiratory failure, while reducing their respiratory effort.
What are the main medical indications for using NIV?
NIV is primarily recommended in cases of acute respiratory failure, particularly for patients with chronic obstructive pulmonary disease (COPD), cardiogenic pulmonary edema, or other respiratory failures accompanied by acidosis. It helps to reduce the work of breathing, limit the need for intubation, and improve gas exchange, which contributes to a better prognosis.
What are the contraindications and possible risks associated with NIV?
NIV is contraindicated in certain cases, particularly in the presence of altered consciousness, a high risk of aspiration, facial trauma, hemodynamic instability, airway obstruction, or excessive secretions. Among the possible risks are aspiration, gastric bloating, pneumothorax, and delayed intubation if NIV fails.
How is an NIV session set up and monitored?
The setup of NIV begins with the selection of a mask and appropriate settings, generally in a hospital setting. Patient and caregiver education is also provided. At home, NIV is installed with precise parameter monitoring, follow-up via questionnaires, regular adjustments, and nighttime recordings. Patient tolerance and respiratory efficiency are periodically assessed to adjust the treatment if necessary.




