Central venous catheters (CVCs) play an important role in accessing the central venous system, particularly in patients requiring prolonged treatments such as chemotherapy, parenteral nutrition, or antibiotic therapy. These devices, inserted into large veins (internal jugular, clavicular, femoral), ensure high venous flow thanks to their precise positioning at the junction of the superior vena cava and the right atrium. Inserting a central venous catheter is a delicate procedure, performed under radiological guidance for optimal placement. It requires strict aseptic technique and constant monitoring to prevent complications such as infection or thrombosis. For nurses, mastering insertion techniques, associated care, and recognizing risk situations is essential for patient well-being.
This guide details the key principles of central venous catheters (CVCs, port catheters, implantable catheters), insertion techniques, and the skills required for effective use in hospital or home settings.
Fundamental Principles of Central Venous Catheters
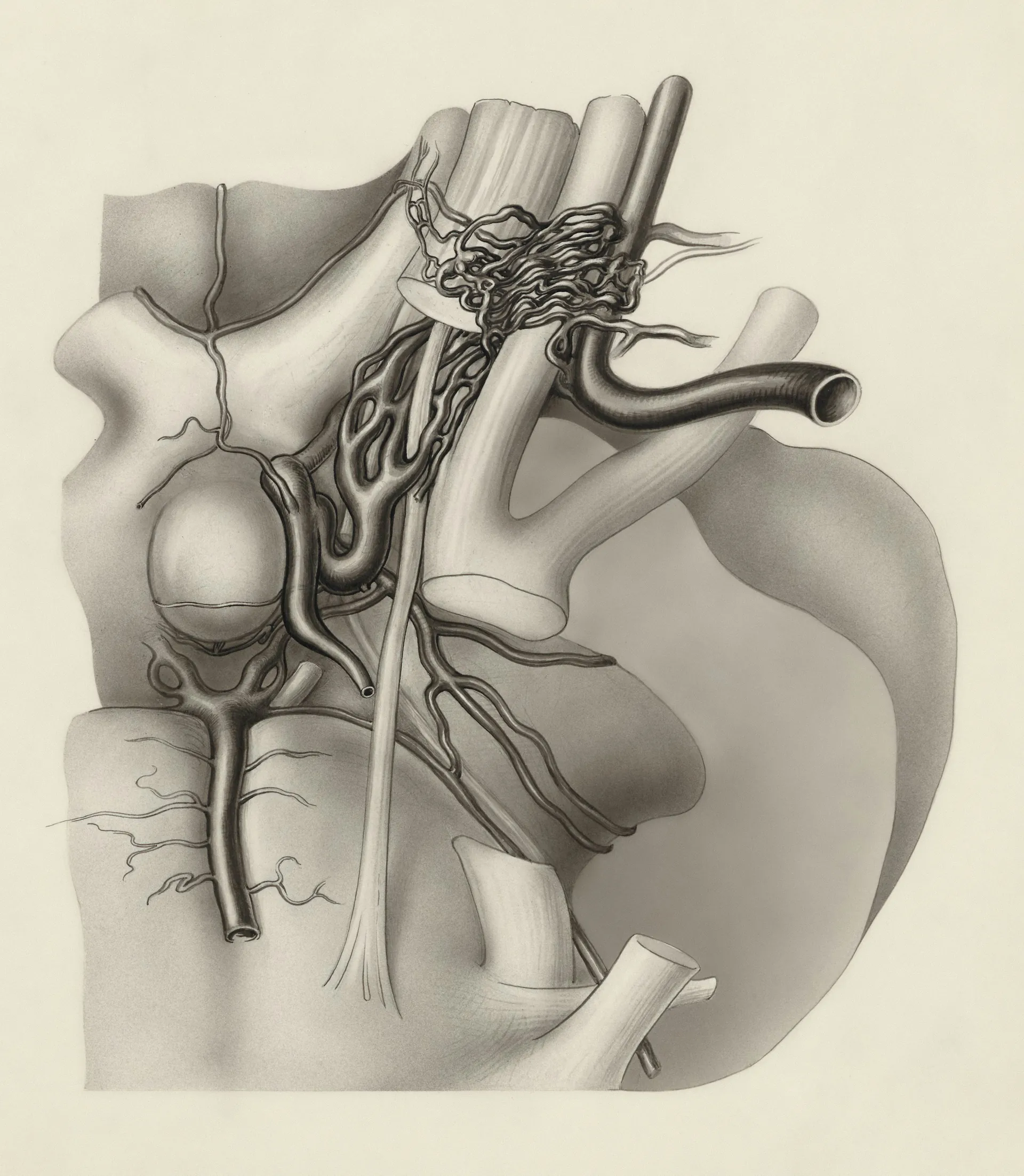
Anatomical and Physiological Understanding
Central venous access uses large-bore veins, such as the internal jugular vein, subclavian vein, or femoral vein, to insert a central venous catheter. These central veins connect to the superior vena cava, carrying blood directly to the right atrium of the heart. This configuration allows for rapid and efficient administration of treatments. The size and depth of these veins, combined with the near absence of valves, facilitate both the passage and correct positioning of the central catheter, while reducing the risk of obstruction. A thorough understanding of this anatomy is essential to ensure proper catheter placement and minimize complications related to its use. Clinical Indications: Central venous catheter placement is indicated in many major clinical situations. Among these indications are:
- The administration of chemotherapy in cancer patients.
- Parenteral nutrition requiring a durable device.
- Prolonged antibiotic treatments.
- Monitoring of central venous pressures or rapid, large-volume infusions.
It is also recommended in cases where peripheral venous access is difficult or impossible to use, or for certain repeated blood draws. Each indication must be subject to a rigorous risk-benefit assessment by the healthcare team.
Risks and complications
Despite their usefulness, central venous catheters present risks that it is essential to know and prevent. Catheter-related infections are the most frequent and feared complication, with the potential to progress to serious systemic infections. Other risks include: Venous thrombosis associated with the presence of the catheter. The risk of pneumothorax during subclavian vein puncture. Cardiac arrhythmias if the catheter is incorrectly positioned. To minimize these complications, rigorous monitoring of the insertion site, meticulous aseptic technique, and routine radiological monitoring are essential. Types of Central Venous Access: PICC Line A PICC line, or peripherally inserted central catheter, is inserted into a deep vein in the arm, usually above the elbow crease, such as the basilic or cephalic vein. This type of central venous catheter is guided to the cavoatrial junction, ensuring reliable access for long-term infusions, often up to six months. It may be equipped with one or more lumens and is held in place by a fixation system such as the Stat-Lock or Grip-Lock. The dressing must be changed regularly and under sterile conditions to minimize the risk of infection.
Implantable Port (Port-a-Cath)
The implantable port, also called a Port-a-Cath, is a type of central catheter fully implanted under the skin. It consists of a metal reservoir connected to a central venous catheter inserted into a central vein such as the internal jugular vein or the subclavian vein. This device is particularly valued for its discretion and comfort, offering long-lasting central venous access without requiring daily care at an exposed insertion site. It is frequently used in oncology for chemotherapy or parenteral nutrition, thus reducing the risk of access site infections. Peripherally Inserted Central Catheter (PICC or Broviac) The tunneled peripherally inserted central catheter, commonly called a Broviac (but also Hickman or Groshong depending on the model), is a tunneled central venous catheter. It is inserted into central veins such as the internal jugular vein or the subclavian vein. This type of catheter is designed for prolonged treatments, with part of the device passing under the skin before reaching the central vein, which reduces the risk of infection at the entry point. It is widely used in pediatrics and for patients requiring intensive and prolonged treatments, such as certain chemotherapy or parenteral nutrition protocols. Insertion and Care Techniques
Sterile Insertion Technique
The insertion of a central venous catheter must be performed under strictly sterile conditions to minimize the risk of infection. This involves thorough handwashing with an alcohol-based hand rub, wearing sterile gloves, a mask, a gown, and a surgical cap. The puncture site is prepared with a rigorous 5-step antiseptic procedure, including application of a suitable antiseptic and complete drying. The use of a sterile drape is essential before insertion, which is often performed under ultrasound guidance and radiological control. Orienting the needle bevel at approximately 10-30 degrees upon vein penetration allows for precise insertion and minimizes venous trauma. Dressing Management: The dressing at the insertion site must be applied using strict aseptic techniques. After each procedure, the old dressings should be carefully removed, a new antiseptic treatment performed using a center-to-peripheral motion, and then a sterile, transparent, semi-permeable dressing applied. This type of dressing allows for visual monitoring of the central venous site without frequent removal. The frequency of dressing changes depends on the established protocol but should not be too frequent to limit contamination, except in cases of signs of infection or detachment. Administration of Medications and Solutions: Administration via a central catheter requires connection to a sterile closed system, often using a safety connector. The lines must be systematically flushed before and after administering solutions, using sterile 0.9% NaCl syringes, to prevent clot formation and maintain patency. Some multi-lumen catheters allow for the simultaneous co-administration of incompatible treatments. Rigorous flow control, correct identification of the pathways, and adherence to infusion protocols are essential for patient safety. Preventing healthcare-associated infections relies on a set of strict measures: handwashing before any manipulation, careful antisepsis of the site and connections, use of sterile equipment, and minimizing the number of openings in the venous circuit. Regular monitoring of the insertion site to detect redness, pain, exudate, or swelling is fundamental. In case of suspected infection, the medical team must be alerted early, and appropriate tests performed, including catheter cultures. Continuing education and adherence to best practices are essential to reduce the risk of infection and ensure optimal health for patients with central venous catheters.
Communication with Patients

Explanation of Procedures
It is essential Take the time to clearly explain to patients the nature and procedure of central venous catheter insertion. By detailing the different steps, the medical reasons justifying this intervention, as well as the benefits and potential associated risks, you help to establish a climate of trust. An explanation adapted to their level of understanding also helps to reduce their anxiety and prepare them mentally for the procedure. Managing Expectations and Concerns: Patients with central venous catheters may have legitimate questions about pain, limitations in their daily activities, or the risk of infection. Your role is to listen attentively to their concerns, answer their questions with empathy, and provide clear and factual information. By communicating transparently, you help the patient to better manage their expectations and to collaborate more actively in their care pathway.
Home care education
A significant part of preventing complications relies on educating the patient about home care. It is essential to teach them how to recognize the signs of infection or catheter malfunction, the need to avoid any unauthorized manipulation of the device, and good hygiene practices. Informing the patient about the importance of attending scheduled check-ups and reporting any abnormalities helps improve the effectiveness of follow-up and ensures the safety of patients with a central venous catheter. Specific skills for using different routes: Role in parenteral nutrition. Parenteral nutrition requires reliable central venous access capable of supporting the long-term infusion of hyperosmotic solutions. Devices such as tunneled central venous catheters (CVCs), PICC lines, or implantable ports like Port-a-Cath are preferred for this function. Their secure implantation and rigorous maintenance are essential to prevent complications such as thrombosis or infection. These devices ensure continuous and appropriate delivery of essential nutrients to the patient, particularly when the digestive tract is compromised or impassable. Role in Chemotherapy: In cancer treatments, central catheters play a fundamental role. They allow the administration of cytotoxic drugs, often corrosive, which require stable, deep, and sustained venous access. This helps reduce the risk of complications such as phlebitis.
Implantable ports, such as Port-a-Cath, are particularly valued for their comfort and discretion, making repeated infusions less burdensome for the patient. Mastering the specifics of these devices, from insertion to removal, is essential to ensure safe and effective care for cancer patients.
Role in Chronic Pain Management
Central venous access is also essential in the management of severe chronic pain. It facilitates the continuous or intermittent administration of potent analgesics. Thanks to central venous access, controlled infusions allow for optimal pain control in patients suffering from refractory pain, while avoiding multiple peripheral venipunctures. To ensure appropriate care, nurses must be familiar with the specific features of these catheters, particularly for adjusting dosage, preventing potential complications, and providing personalized follow-up for each patient. Conclusion: Central venous access is an essential device in nursing care. It allows for the administration of complex treatments such as chemotherapy, parenteral nutrition, and the management of chronic pain. Their placement and maintenance require a thorough knowledge of anatomy, the use of rigorous sterile techniques, and constant vigilance to prevent the risk of infection. As a nurse, mastering these specific skills is essential to guarantee the safety and comfort of your patients. Don't hesitate to deepen your knowledge and meticulously apply best practices to optimize the quality of care.
FAQ
What are the main indications for inserting a central venous catheter?
Inserting a central venous catheter is primarily indicated for the administration of intensive and prolonged treatments such as:
- Chemotherapy
- Parenteral nutrition
- Long-term antibiotic therapy
- Administration of blood or blood products
- Pressure monitoring
- Rapid fluid resuscitation
- Cases of impossible or difficult peripheral venous access
To handle a central venous catheter, it is essential to maintain rigorous hygiene:
- Wash your hands thoroughly
- Wear sterile gloves
- Use sterile equipment
- Disinfect the site with chlorhexidine alcohol
It is important to avoid any resistance during injection, to handle the devices gently, and to monitor for signs of infection.
The dressing must remain aseptic and be changed according to the current protocol.




