Biological risk in healthcare facilities refers to threats posed by biological agents such as viruses, bacteria, fungi, or parasites. These can cause serious infections in patients and staff, particularly in environments characterized by invasive medical procedures and the presence of infectious diseases, such as during epidemics like COVID-19.
It is essential to understand, assess, and control these risks to limit the transmission of pathogens, protect healthcare workers, and ensure health safety.
This involves strict hygiene measures, the use of personal protective equipment, secure management of infectious waste, as well as ongoing training and regular evaluation of professional practices. Under the supervision of occupational health physicians, these actions effectively reduce exposure to biological agents and strengthen occupational health. Understanding biological risk in healthcare facilities: What is a biological risk? A biological risk refers to the threat to workers' health due to exposure to biological agents, such as viruses, bacteria, fungi, prions, or parasites, which can cause infectious diseases. These biological agents are classified into groups according to their hazard, their ability to spread in the community, and the existence of appropriate treatments or preventive measures.
Biological risk materializes as the potential contamination of professionals through various modes of transmission, such as blood contact, airborne transmission, or skin contact. This risk concerns both intentional exposures in the laboratory and accidental exposures in the workplace.
Sources of Biological Risk in Healthcare Facilities
In healthcare facilities, there are numerous sources of biological risk. These include contact with infected patients, handling biological samples, managing infectious medical waste, and using sharp objects such as needles. Blood, bodily fluids, secretions, and contaminated surfaces constitute natural reservoirs of pathogens. The chain of transmission can occur through exit points (e.g., wounds, sputum) and then entry points (e.g., punctures, mucous membranes), directly exposing the biologically sensitive worker. The Importance of Prevention Against Biological Risks: Prevention is essential to limit exposure to biological risks and protect the health of both healthcare workers and patients. Appropriate measures — based on a rigorous assessment of the biological risks associated with the work situation — make it possible to break the chain of transmission. Prevention includes strict hygiene, individual and collective protection, secure management of infectious waste, and mandatory vaccination when required. It is also part of a comprehensive approach involving training, raising awareness of occupational risks, and the active role of occupational health services and the occupational physician.
The most common pathogens in hospitals
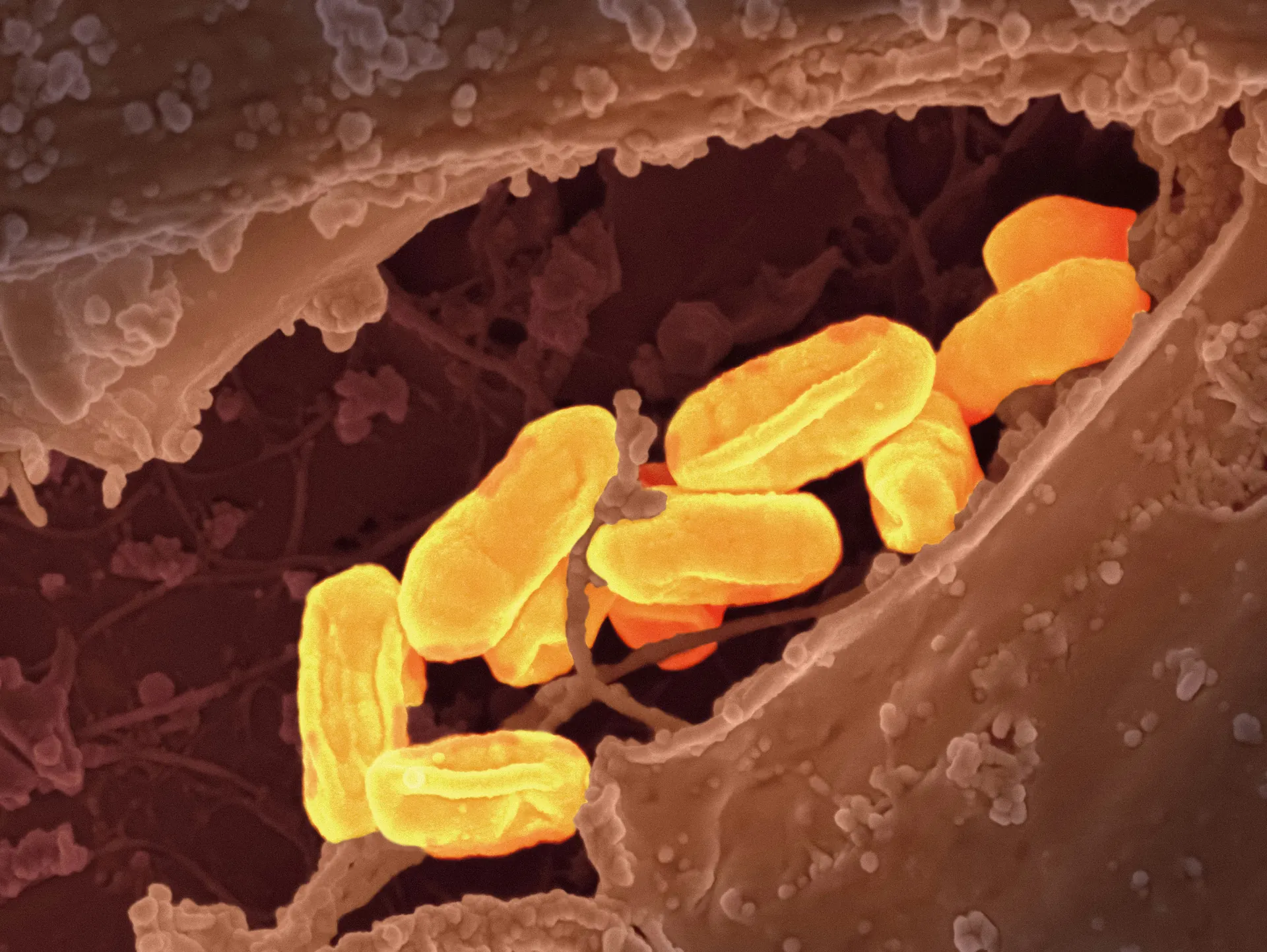
In hospitals, bacteria and viruses are the biological agents most frequently involved in infectious risks. Among bacteria, certain species such as methicillin-resistant Staphylococcus aureus (MRSA), Escherichia coli, and Klebsiella pneumoniae are of particular concern due to their high prevalence and increasing resistance to antibiotics. On the viral side, we find those responsible for respiratory infections, such as SARS-CoV-2, as well as hepatitis B and C viruses, which are often linked to exposure to blood and sharp objects.
The diversity and virulence of these biological agents considerably complicate their control in healthcare facilities.
Antimicrobial resistance: a growing challenge
Antimicrobial resistance represents a major challenge in the management of biological risks in hospitals. The frequent, and sometimes excessive, use of antibiotics contributes to the emergence of multidrug resistant (MRE) pathogens, making some infections extremely difficult to treat. These resistant bacteria thrive particularly in hospitals, where the high concentration of immunocompromised patients facilitates their transmission. Infections caused by these multidrug-resistant agents lead to increased morbidity, higher medical costs, and complicate the implementation of prevention and treatment strategies. Nosocomial infections: a major public health challenge. Nosocomial infections, contracted during hospital stays or medical procedures, represent a major public health challenge. In France, it is estimated that more than 150,000 cases occur each year, with serious consequences for patients' health and a significant number of deaths. These infections are often associated with invasive procedures and the use of medical devices such as catheters or probes. Combating these infections requires constant vigilance, continuous assessment of occupational biological risks, and the implementation of rigorous preventive measures in all healthcare departments.
Strategies for the Prevention and Control of Biological Risks

Hygiene and Disinfection
Hygiene protocols in healthcare facilities play a central role in preventing biological risks. They rely on rigorous cleaning of surfaces and equipment near patients. This process combines the physical removal of soiling and the application of appropriate disinfectants to neutralize pathogens.
Bio-cleaning takes place in several successive stages: cleaning, rinsing, and then disinfection using specific detergent-disinfectant solutions. Innovative methods, such as disinfection by high-temperature steam, are also used to ensure effective cleaning while reducing the use of harsh chemicals.
These protocols must be scrupulously followed and regularly monitored to adapt to the evolution of biological agents and effectively limit the transmission of infections.
Management of Infectious Healthcare Waste (DASRI)
The secure management of infectious healthcare waste (DASRI) is an essential component of biological risk prevention in hospitals. This waste, including needles, soiled dressings, or any material that has come into contact with biological fluids, must be collected, sorted, packaged, and disposed of according to strict procedures. The goal is to prevent any accidental exposure to pathogens, particularly for workers handling this waste and cleaning staff. Specific devices and appropriate training are implemented to ensure disposal complies with health and safety standards. Personal Protective Equipment (PPE): An Essential Barrier. Personal protective equipment (PPE) is essential to protect healthcare professionals exposed to biological agents. It includes gloves, gowns, masks, protective eyewear, and face shields, forming an effective barrier against splashes, direct contact, or aerosols. The choice of PPE is adjusted according to the type of risk identified and the activities carried out. Thorough training is necessary to ensure their correct fitting and use, as unsuitable or improperly used protection can compromise their effectiveness. Strict adherence to procedures for donning, doffing, and storing PPE is fundamental to limit exposure and prevent occupational risks related to biological agents.
Training and awareness of healthcare personnel

The importance of continuing education
Emergency Procedure Simulation and Training
Simulations and practical training in emergency procedures play a key role in preparing teams to react quickly and effectively to an accident involving exposure to biological agents, such as an accidental needle stick or a spill of contaminated material. These exercises allow for the practical application of first aid techniques, mastery of isolation and decontamination protocols, and improved coordination between different professionals. Regular repetition of these drills promotes an organized response and minimizes the risk of contamination in critical situations. A strong safety culture in healthcare facilities is essential for all healthcare professionals to make a lasting commitment to biological risk prevention. This culture is based on transparent communication, the sharing of best practices, the empowerment of each professional, and the implementation of clear and accessible procedures.
Fostering an environment where the reporting of incidents and near misses is encouraged allows for continuous evaluation of practices and improvement of protective measures.
The safety culture thus strengthens collaboration between teams for a safer work environment and better patient care.
Roles and responsibilities in biological risk management

The Role of Infection Prevention and Control Services
Infection prevention and control services play a central role in managing biological risks within healthcare facilities. They are responsible for the development, implementation, and monitoring of protocols aimed at limiting the transmission of biological agents. These services also conduct regular assessments of occupational exposures and coordinate the necessary corrective actions. Their mission includes ongoing staff awareness training, monitoring of hospital-acquired infections, and developing strategies tailored to each department, in collaboration with hospital hygiene experts. This proactive approach helps reduce risks and protect both patients and healthcare workers. Management Commitment and Safety Policy: Management commitment is a key element in implementing an effective biological risk management policy. Management must define clear objectives, allocate the necessary resources, and promote a safety culture within the institution. It also ensures compliance with regulatory obligations, such as risk assessments and mandatory vaccinations when required. Thanks to its support, management facilitates communication between departments, encourages continuing education, and promotes the reporting of incidents related to biological exposures. This coordinating role guarantees a comprehensive, consistent, and sustainable prevention policy. Collaboration between different healthcare professionals: Biological risk management relies on close collaboration between occupational physicians, nurses, biologists, technicians, and cleaning staff. Although each professional has specific responsibilities, coordination between these stakeholders is essential to ensure effective risk control. Sharing information, implementing joint procedures, and maintaining collective vigilance allow for the continuous adaptation of protective measures. This synergy not only strengthens the safety of exposed staff, but also the quality of care provided to patients.
Monitoring, evaluation and improvement of practices
Nosocomial infection surveillance systems
Audit and Feedback: Tools for Continuous Improvement
Auditing professional practices, combined with constructive feedback, plays a crucial role in the continuous improvement of prevention measures. These audits examine compliance with hygiene protocols, the management of personal protective equipment, and the sorting of infectious waste.
Gap analysis highlights weaknesses and enables the implementation of appropriate corrective actions. Feedback to the teams involved encourages awareness, the adoption of best practices, and strengthens collective commitment to reducing occupational biological risks. The impact of new technologies on prevention: New technologies offer major advances in the prevention of biological risks. Innovative solutions, such as automated sterilization systems, computerized traceability of infectious medical waste, and smart sensors for monitoring hand hygiene, contribute to increased safety. Furthermore, digital platforms simplify distance learning, facilitate the collection and analysis of monitoring data, and improve communication between the various stakeholders. The integration of these technologies optimizes risk management while meeting increasing occupational health and safety requirements.
Conclusion
Managing biological risks in healthcare facilities requires a rigorous approach that combines assessment, prevention, training, and collaboration among professionals. Adherence to hygiene protocols, appropriate use of personal protective equipment, and secure management of infectious waste are essential for reducing exposure risks.
Constant monitoring and regular audits play a key role in improving practices. Faced with these challenges, it is essential that each stakeholder takes responsibility and that healthcare facilities actively invest in implementing concrete measures to guarantee the safety and health of all.
FAQ
What is biological risk in healthcare facilities and what are its main sources?
Biological risk in healthcare facilities represents a threat to the health of staff, linked to exposure to pathogenic biological agents such as viruses, bacteria, fungi, or prions.
The main sources include blood, biological fluids, contaminated waste, air, and surfaces soiled by these agents.
What are the key prevention measures to limit exposure to biological risk in hospitals?
To reduce exposure to biological risk in hospitals, it is essential to implement measures such as isolating contagious patients, improving ventilation, regularly disinfecting surfaces, using personal protective equipment, providing ongoing staff training, ensuring safe waste management, and monitoring by a dedicated infection prevention team.
How can biological risks be assessed and prioritized to better control them in a hospital setting?
Assessing and prioritizing biological risks requires identifying reservoirs of biological agents and exposure activities. Next, the probability and severity of contamination should be analyzed according to the transmission routes. This approach allows for the establishment of priorities and the implementation of appropriate preventive measures. What should you do in case of accidental exposure to a hazardous biological agent during patient care or in the laboratory? In case of accidental exposure to a hazardous biological agent, it is imperative to immediately rinse the affected area with water or saline solution, cover the wound, and then report the incident without delay. The appropriate post-exposure prophylaxis protocol must be followed, which often includes preventive medication, and a doctor must be consulted promptly.




