Hemovigilance is an essential system designed to guarantee transfusion safety throughout the entire process, from blood collection to transfusion to the patient. It relies on the monitoring and evaluation of adverse effects that may occur during the therapeutic use of labile blood products (LBP), such as red blood cell concentrates, platelets, or plasma.
This complex transfusion chain, which extends from donors to healthcare facilities, is based on a strict system of screening, quality control of blood products, and risk management.
Hemovigilance plays a key role in enabling the identification, reporting and prevention of adverse effects related to transfusions. It is coordinated nationally by organizations such as the National Agency for the Safety of Medicines and Health Products (ANSM) and the French Blood Establishment (EFS).
This comprehensive guide is designed for healthcare professionals who wish to better understand and master this system, guaranteeing the health and safety of both recipients and donors.
What is hemovigilance?
Definition and objectives
Hemovigilance is an organized surveillance system that covers the entire transfusion chain, from blood collection to the monitoring of recipient patients. Its main objective is to prevent, detect, report, and analyze any adverse effect or incident related to the use of labile blood products. It aims to ensure transfusion safety by guaranteeing the quality and reliability of the products, while protecting the health of recipients and donors.
Thanks to this system, hemovigilance allows for continuous monitoring of adverse effects that may occur during blood transfusion. It also plays a key role in implementing corrective measures to reduce the risks associated with transfusion.
History and Importance of Hemovigilance
Hemovigilance emerged in the 1990s in response to serious transfusion incidents and health crises related to blood safety, particularly the transmission of infectious diseases. In France and elsewhere, this system has become a cornerstone of the surveillance and evaluation of transfusion-related adverse events. It relies on the collaboration of institutional actors such as the National Agency for the Safety of Medicines and Health Products (ANSM) and the French Blood Establishment (EFS). Its development has considerably strengthened the safety and confidence in the use of blood products. It has also enabled the introduction of advanced screening and traceability practices, thanks to rigorous management of labile blood products (LBP). This system is now essential to guarantee public health. It ensures constant vigilance regarding the risks associated with blood components and their therapeutic use.
The actors in hemovigilance
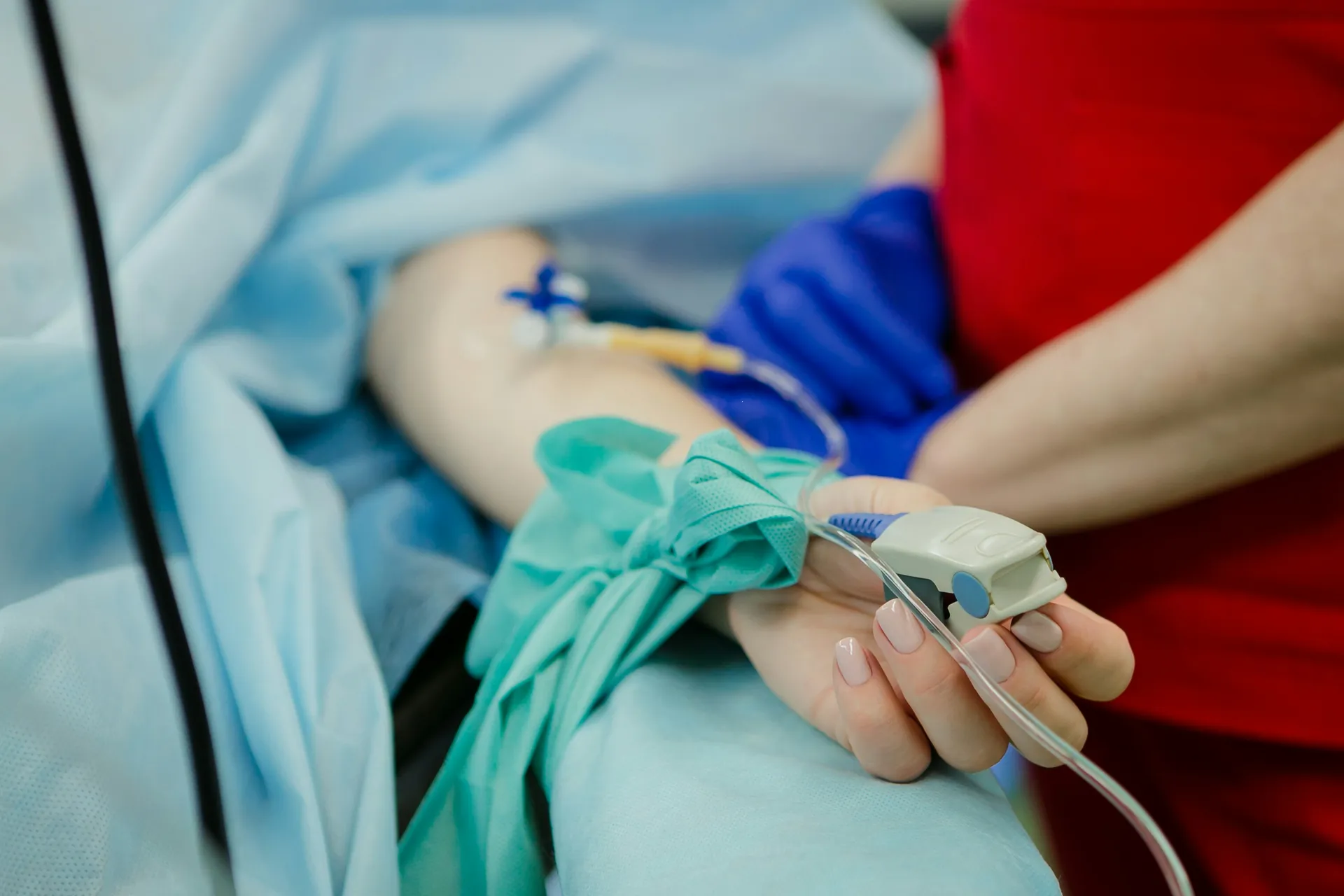
Roles and responsibilities within healthcare facilities
At the heart of the organization of In hemovigilance within healthcare facilities, several actors play specific and complementary roles. The hemovigilance correspondent, designated in each public or private healthcare facility, is responsible for collecting and reporting any adverse effect occurring in a recipient of labile blood products, as well as any serious incident related to the transfusion chain. He manages the investigations and ensures compliance with hemovigilance procedures. Healthcare professionals play an active role by reporting incidents or adverse effects to the hemovigilance correspondent without delay. Furthermore, the transfusion safety and hemovigilance committees, present in public institutions, ensure the implementation of corrective and preventive measures.
Finally, the regional hemovigilance coordinator intervenes at the regional level, in collaboration with the regional health directorates, to guarantee the consistency and monitoring of actions at the local level.
Partnerships with blood transfusion organizations
Hemovigilance also relies on close collaboration with blood transfusion organizations, primarily the French Blood Establishment (EFS). The latter provides labile blood products, participates in quality control and screening of donors. Hemovigilance officers at transfusion centers report any serious adverse event in a donor or any incident in the transfusion chain to the ANSM (French National Agency for Medicines and Health Products Safety). This collaboration is essential to guarantee traceability and safety throughout the transfusion chain. The ANSM, as the national reference body, coordinates and supervises the entire system at the national level. This strong partnership between institutional actors and healthcare facilities ensures a rigorous and effective hemovigilance system.
Products covered by hemovigilance
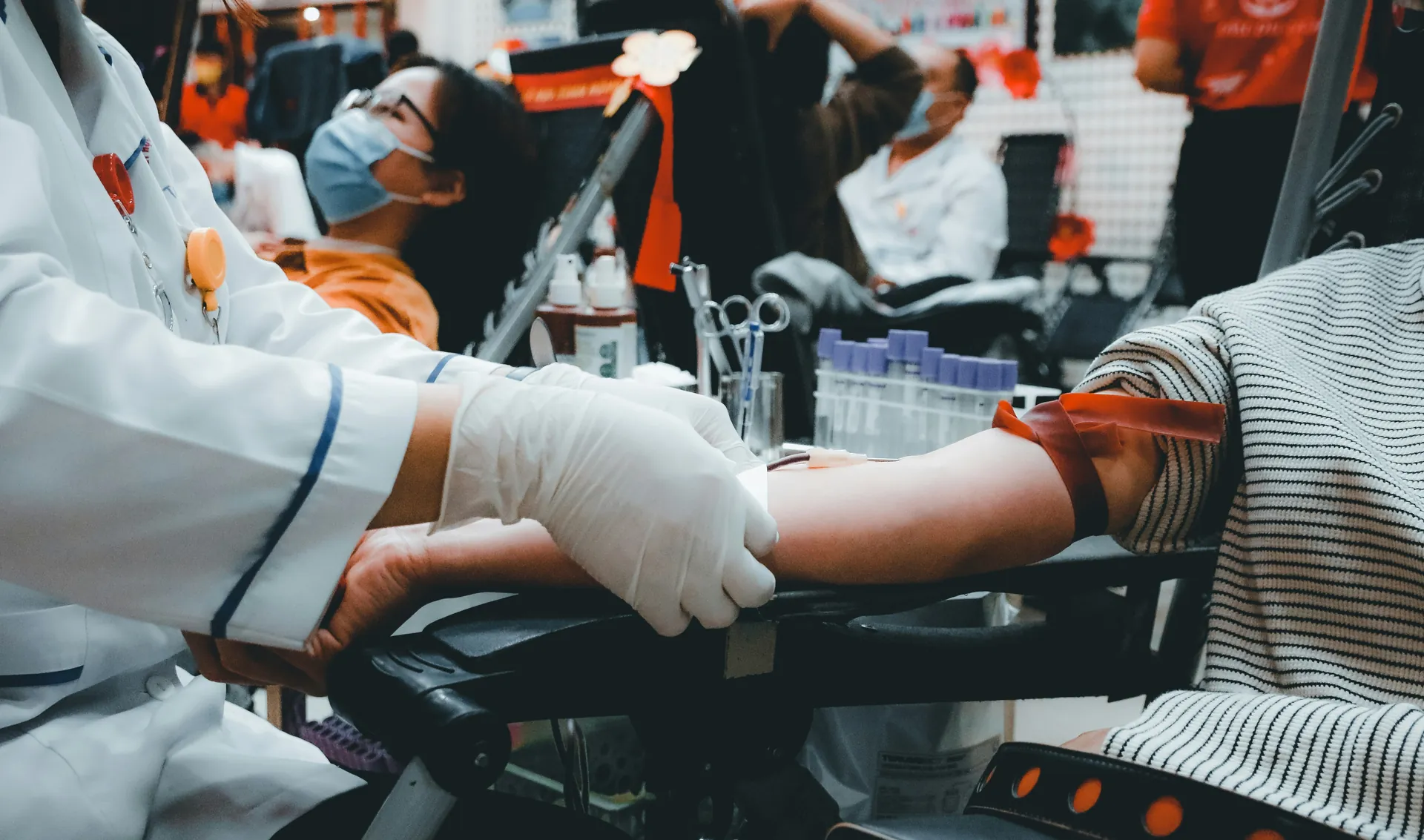
The different labile blood products
Labile blood products (LBP) include several types of components derived from blood donation, each with specific characteristics and therapeutic indications. Among them, the main distinctions are:
- Red blood cell concentrates (RBCs), used to correct anemias by delivering oxygen to tissues.
- Platelet concentrates (PCs), intended to restore hemostasis in patients suffering from thrombocytopenia or platelet dysfunction.
- Fresh frozen plasma (FFP), used to treat coagulation disorders by providing essential plasma factors.
- Mixed granulocyte concentrates, used less frequently for certain specific cases of severe immunosuppression.
These products are subject to numerous qualifications, such as
- Leukoreduction, to reduce immune reactions.
- Rigorous batch traceability.
- Product qualification to prevent complications such as alloimmunization or the transmission of infectious agents.
Continuous monitoring via hemovigilance allows for the identification and control of adverse events occurring after transfusion, thus ensuring constant improvement in transfusion safety for the benefit of the patient.
The hemovigilance reporting procedure
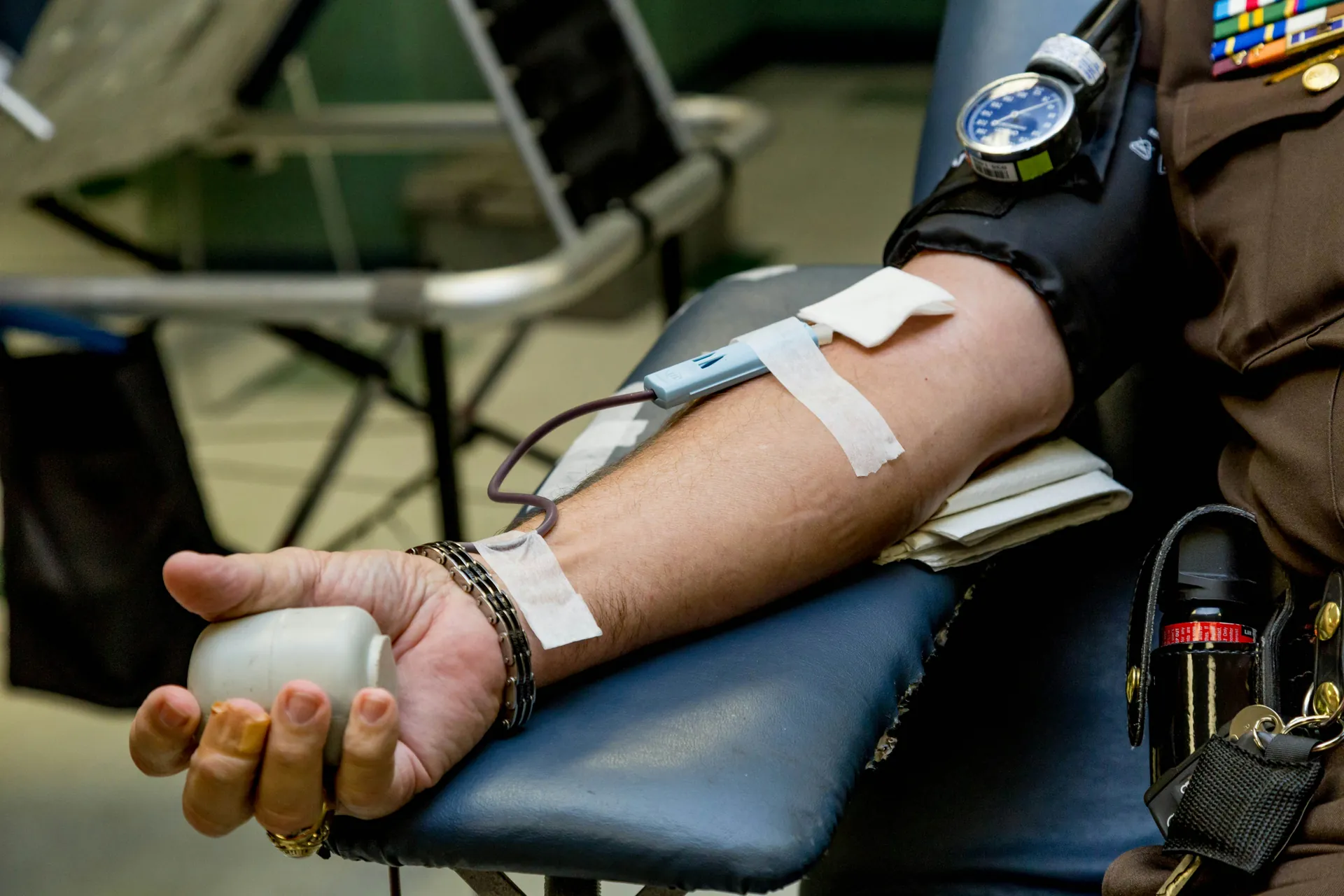
Identification and management of transfusion incidents
The hemovigilance reporting procedure begins with the rigorous identification of any incident or adverse effect occurring in a patient receiving labile blood products. It is imperative that all healthcare professionals immediately report any adverse event, particularly serious incidents, to their institution's hemovigilance officer.
These officers, often physicians or pharmacists, are responsible for managing and analyzing reported cases. They conduct thorough investigations, which may include further tests, to determine the cause of the incident. Reports are submitted via the e-FIT online reporting application and then forwarded to the regional hemovigilance coordinator, the ANSM (French National Agency for Medicines and Health Products Safety), and the French Blood Establishment (EFS).
Reporting deadlines vary depending on the severity of the incidents, some of which must be reported urgently. This procedure allows for a better risk assessment and facilitates the development of appropriate corrective measures to prevent the recurrence of adverse effects related to transfusions.
The Importance of Blood Product Traceability
Traceability is an essential element in the transfusion chain and plays a key role in the safety of transfusion procedures. It guarantees precise tracking of each unit of blood product, from its collection from the donor to its administration to the patient. Each step is meticulously documented, encompassing identification checks, storage and transport conditions, as well as the delivery of products to healthcare facilities. This traceability is essential not only to ensure the quality and safety of labile blood products, but also to enable a rapid response in the event of an incident or adverse effect. It thus facilitates the investigation of causes and the management of consequences. Furthermore, it constitutes a regulatory obligation for all actors in blood transfusion, contributing to increased vigilance and the continuous improvement of transfusion safety.
Risk Management and Prevention Practices
Risk Assessment Related to Transfusion
Risk assessment in blood transfusion is an essential step to guarantee transfusion safety. It is based on a systematic analysis of potential hazards throughout the transfusion chain, from collection from donors to administration to patients.
This assessment includes the identification of infectious and immunological risks, as well as procedural or compatibility errors.
Specific methods, such as FMEA (Failure Mode and Effects Analysis), are used to detect system weaknesses and prioritize the necessary corrective actions. The goal is to prevent and reduce as much as possible the adverse effects associated with transfusions, while ensuring optimal quality of the labile blood products used in transfusion therapy. Prevention and Management of Adverse Effects: Hemovigilance prevention practices are based on rigorous protocols validated by the French National Agency for Medicines and Health Products Safety (ANSM). Key measures include thorough screening for infectious agents in donors, biological qualification of blood products, and ongoing training for medical teams to ensure safe administration. In the event of a transfusion-related adverse event, rapid and coordinated management is essential. This includes immediate reporting to the hemovigilance officer, appropriate patient management, and rigorous medical follow-up to prevent any recurrence.
These steps, combined with continuous vigilance and regular audits, help to reduce incidents and strengthen the overall quality of transfusion care.
Hemovigilance Training and Awareness
Training Programs for Healthcare Professionals
To guarantee quality and transfusion safety, specialized training programs are available to healthcare professionals involved in the transfusion chain. These training courses offer the opportunity to update knowledge on labile blood products, compatibility rules, and the recognition and management of transfusion-related adverse events. They also cover the regulatory requirements defined by the French National Agency for Medicines and Health Products Safety (ANSM) and delve deeper into the organization of hemovigilance. Structured around theoretical and practical modules, these courses are designed for a wide range of professionals, such as physicians, nurses, pharmacists, and other healthcare personnel. They are often validated by certifications such as the CPD (Continuing Professional Development).
A central point of these training courses is to emphasize the importance of the role of the hemovigilance officer and to promote essential best practices for reducing transfusion-related risks.
Implementation of awareness campaigns
In addition to training, hemovigilance awareness is part of an ongoing process within healthcare facilities. Targeted information campaigns are regularly organized to remind healthcare professionals of reporting procedures, the importance of traceability of blood products, and the actions to take in case of an adverse event. These campaigns utilize a variety of media, including posters, newsletters, and practical workshops. Their objective is to encourage the involvement of all healthcare teams. By cultivating a culture of vigilance and shared responsibility, these initiatives help strengthen transfusion safety and maintain the trust of donors and patients.
Tools and resources available for professionals

Hemovigilance Guides and Protocols
Healthcare professionals have access to numerous guides and hemovigilance protocols to ensure rigorous and safe management of blood transfusions. These documents provide clear recommendations on the procedures to follow, from prescription to the management of potential adverse effects.
They specify, in particular, the essential steps of the transfusion procedure, best practices regarding patient identification, traceability of labile blood products, and the procedures to follow in the event of transfusion incidents. These protocols are developed by leading institutions such as the French Blood Establishment (EFS) and the National Agency for the Safety of Medicines and Health Products (ANSM). These organizations ensure a coherent national regulatory framework adapted to the current challenges of transfusion safety. Dedicated IT Support and Software: To simplify data management and improve incident reporting, IT tools specifically designed for hemovigilance are made available to healthcare facilities. This specialized software allows for the rapid collection, analysis, and transmission of information related to incidents and adverse events. Among these tools, the national application e-FIT is widely used for the electronic reporting of recipient adverse event reports. It guarantees secure and standardized transmission of data to the competent authorities. These systems strengthen the complete traceability of the transfusion chain and facilitate coordination between the various stakeholders, from healthcare facilities to the regional hemovigilance coordinator and the ANSM (French National Agency for Medicines and Health Products Safety). Thanks to these technologies, the monitoring and evaluation of transfusion safety are optimized, thus contributing to better risk prevention. Conclusion: Hemovigilance plays an essential role in guaranteeing transfusion safety at every stage of the process, from collection from donors to the monitoring of recipient patients. It is based on increased vigilance, rigorous reporting of adverse effects and close collaboration between healthcare facilities, the French Blood Establishment and the ANSM. To effectively protect all stakeholders, it is essential that each professional actively engages in the application of good hemovigilance practices and participates in dedicated training programs.
Act today to strengthen transfusion health and guarantee the safety of the blood product throughout the entire chain.
FAQ
What is hemovigilance and what is its main role in transfusion safety?
Hemovigilance is a health surveillance system that monitors the entire blood transfusion chain, from blood collection to recipient follow-up. Its main objective is to prevent and assess adverse effects associated with the use of blood products.
What types of adverse events must healthcare professionals report in a hemovigilance system?
In a hemovigilance system, healthcare professionals must report serious adverse events in donors as well as transfusion-related incidents or reactions. This includes:
- Identification errors,
- Inadequate blood products,
- Allergic reactions,
- Alloimmunization,
- Abnormalities related to massive transfusion,
- And any deviation from established protocols.
What are the key steps of the final check to be performed at the patient's bedside before a blood transfusion?
Before a blood transfusion, it is essential to perform a final check at the patient's bedside. Here are the key steps:
- Verification of the patient's identity by questioning or via their wristband,
- Concordance between medical documents and the blood product (phenotypes, number, expiry date),
- Visual inspection of the product and ABO-Rh biological compatibility test by agglutination.
Who is responsible for reporting and managing transfusion-related incidents within a hemovigilance system?
The responsibility for reporting and managing transfusion incidents lies with:
- Healthcare professionals,
- Hemovigilance correspondents,
- And regulatory bodies, such as the ANSM in France.
These actors collaborate closely to report and analyze incidents in order to improve transfusion safety.




