Extracorporeal membrane oxygenation (ECMO) is an advanced medical technique that temporarily supports the functions of the heart and lungs. By extracting and reoxygenating blood outside the body, this sophisticated system provides essential respite for these vital organs, promoting their recovery from serious illnesses. Frequently used in cases of acute respiratory distress, severe heart failure, or post-surgical complications, ECMO is a proven and life-saving solution, particularly in critical situations such as ARDS or COVID-19. This method also raises questions about its benefits and limitations, and is the subject of ongoing research. In intensive care units, it is a valuable tool, guiding teams in complex situations and increasing patients' chances of survival. ECMO, although technically demanding, remains an essential pillar of modern life support.
What is ECMO?
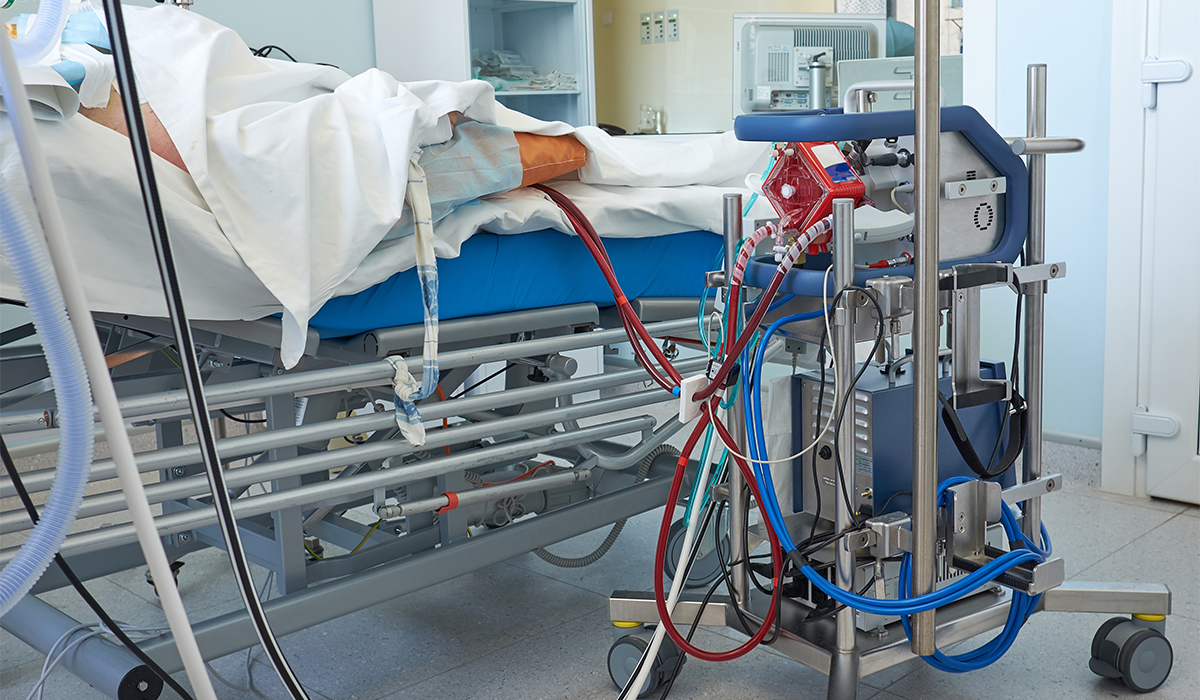
Definition and Functioning
Extracorporeal membrane oxygenation (ECMO) is a circulation technique Extracorporeal membrane oxygenation (ECMO) provides simultaneous cardiac and respiratory support to patients whose heart and/or lungs cannot maintain sufficient gas exchange to sustain life. This procedure simulates the vital functions of the heart and lungs by removing deoxygenated blood, passing it through a special membrane that removes carbon dioxide and injects oxygen, before returning it to the bloodstream. The process involves inserting cannulas into blood vessels to extract blood, which is then pumped through a membrane oxygenator. This oxygenator mimics the function of the lung alveoli by removing carbon dioxide and adding oxygen. Once oxygenated, the blood is warmed and then returned to the body. To prevent clotting in the extracorporeal circuit, systemic anticoagulation is necessary. In addition, antibiotic prophylaxis is frequently administered to reduce the risk of infection. The two main forms: VV-ECMO and VA-ECMO. ECMO comes in two main modes: veno-venous (VV-ECMO) and veno-arterial (VA-ECMO). VV-ECMO is used specifically to provide respiratory support. In this context, blood is drawn from the venous system, oxygenated outside the body, and then returned to the venous system. This method is particularly suitable for patients with acute respiratory distress, such as in acute respiratory distress syndrome (ARDS). Cannulas are typically inserted into large veins, such as the internal jugular and femoral veins, and oxygenated blood is redistributed to the right atrium to be pumped by the heart to the lungs. VA-ECMO, on the other hand, provides both cardiac and respiratory support. In this configuration, blood is drawn from the venous system, oxygenated, and directly returned to the arterial system. This method is used in patients with severe heart failure or a combination of cardiac and respiratory failure. Cannulas for VA-ECMO are typically inserted into a large vein and artery, such as the femoral vein and carotid artery. This technique allows the system to partially take over the heart's pumping function, enabling it to gradually recover. When does ECMO become a treatment option? ECMO eligibility criteria: ECMO is considered a treatment option when patients have severe respiratory or cardiac failure that may be reversible. Although eligibility criteria may vary between institutions, some universal criteria are commonly adopted.
In the context of acute respiratory distress, patients generally become eligible for ECMO if their PaO2/FiO2 ratio falls below 50 mmHg, despite mechanical ventilation with an FiO2 of 100% and a PEEP greater than or equal to 5 cm H2O. Similarly, refractory hypercapnia accompanied by a pH below 7.25, despite optimized maneuvers (alveolar recruitment and inhaled vasodilators), may also classify the patient as a potential candidate for ECMO. Regarding cases of cardiac support, the indication for ECMO becomes particularly clear in situations of refractory cardiogenic shock, despite optimal medical treatments. Myocardial infarction, acute myocarditis, postpartum cardiomyopathy, or decompensated heart failure may justify this decision. Furthermore, some patients with septic shock, when the cause is identified and initial resuscitation is effective, may also benefit from ECMO.
Limitations and Ethical Considerations
While ECMO can offer a chance of survival in critical circumstances, it is not without limitations and ethical questions. Common exclusion criteria include factors such as extreme age (generally patients under 12 or over 65), lung injuries older than 21 days, pulmonary capillary wedge pressure exceeding 25 mmHg, severe burns, or terminal illnesses with a fatal short-term prognosis. Decisions regarding ECMO also require thorough and collective ethical reflection, particularly when assessing the duration of treatment or deciding to discontinue it. These decisions involve collaboration between physicians, patients, and families, while respecting principles such as beneficence, non-maleficence, and patient autonomy. Complex situations can arise, such as the use of ECMO as a "bridge to nowhere," where the patient is neither eligible for transplantation nor expected to achieve functional recovery, thus creating significant ethical challenges. Furthermore, limited medical resources and complications associated with ECMO are factors to consider. These complications include systemic infections, bleeding or coagulopathic disorders, neurological damage, and limb ischemia caused by catheters. These risks underscore the need for transparent communication and shared decision-making to integrate the multiple complex dimensions of this type of treatment.
ECMO in the fight against critical cases

Use of ECMO in cases of severe acute respiratory distress
ECMO Venous-venous (VV-ECMO) plays a crucial role in the management of severe acute respiratory distress, particularly in acute respiratory distress syndrome (ARDS). This condition, characterized by significant lung inflammation, causes respiratory distress that is refractory to conventional treatments such as mechanical ventilation. ECMO takes over pulmonary function by simultaneously oxygenating and removing carbon dioxide from the body, thus providing valuable time for the lungs to regenerate. Patients receiving VV-ECMO benefit from invasive ventilation, described as "ultra-protective," designed to limit the lung damage often associated with mechanical ventilation. In accordance with the recommendations of the Extracorporeal Life Support Organization (ELSO), the initial parameters include a positive end-expiratory pressure (PEEP) of 15 cmH₂O, an inspiratory pressure of 25 cmH₂O, and a respiratory rate of 5 breaths per minute. These settings can be adjusted according to the patient's response and the need to optimize gas exchange during treatment. ECMO in the context of COVID-19: During the COVID-19 pandemic, ECMO was an essential option for patients with severe forms of ARDS. The disease often led to severe hypoxemia accompanied by respiratory acidosis unresponsive to conventional therapies, making ECMO vital for these critical cases. Data collected during studies, such as those conducted by the Sorbonne University team or the COVID-ICU registry, have demonstrated the effectiveness of ECMO in improving survival rates in these patients. Furthermore, veno-arterial ECMO has been predominantly used, although veno-arterial ECMO (VA-ECMO) has also been applied in certain specific situations. The criteria for ECMO access in this context included severe hypoxemia (PaO2/FiO2 < 150) and/or respiratory acidosis (pH < 7.25 with PaCO2 > 60 mmHg) resistant to conventional mechanical ventilation strategies. ECMO Rescue in Severe Cardiogenic Shock: Veno-arterial ECMO (VA-ECMO) is proving to be an invaluable lifesaving technique for patients suffering from severe cardiogenic shock – failure of the heart muscle preventing sufficient blood flow to meet the body's physiological needs. By temporarily taking over cardiac function and relieving the left ventricle, VA-ECMO allows for better patient management and is associated with id="">optimized clinical results.
It offers medical teams a critical period to intervene more definitively, whether through heart transplantation or other major surgical repairs. However, VA ECMO is not a treatment in itself, but rather acts as an essential bridge towards more long-term therapeutic options or partial or even complete recovery.
Comparison of ECMO approaches with other techniques

Unlike many other life support techniques, ECMO (Extracorporeal Membrane Oxidation) represents an advanced and sometimes decisive approach in the treatment of respiratory and cardiac failure. While this strategy offers significant benefits, it is essential to examine its specific characteristics and compare it with other therapeutic methods to fully understand its advantages and limitations. Mechanical Ventilation: Mechanical ventilation is frequently used to treat patients with acute respiratory distress. However, its prolonged use can lead to lung injury, particularly due to excessively high positive pressures or an inappropriate tidal volume. ECMO, especially in its veno-venous form (VV-ECMO), offers an attractive alternative. It allows for a reduction in ventilation parameters and provides the lungs with a genuine period of rest necessary for their recovery. This minimizes the potential damage induced by conventional mechanical ventilation.
Ventricular Assistance
The use of ventricular assistance devices, such as left ventricular assist devices (LVADs), is primarily reserved for patients with chronic heart failure or those awaiting transplantation. However, these devices do not meet the respiratory needs of these patients.
In comparison, veno-arterial ECMO (VA-ECMO) provides combined support for both cardiac and respiratory functions. This characteristic makes it particularly useful in acute cardiorespiratory failure situations.
Portable Extracorporeal Membrane Gas Exchange
With the emergence of portable ECMO systems, such as the Cardiohelp®, increased flexibility is now possible. These lightweight devices allow for patient transport while maintaining vital stability, particularly between different healthcare facilities.
Studies suggest that these portable devices can reduce transfusion requirements and improve certain clinical outcomes, thus offering a suitable solution in settings where rapid intervention is essential. However, their use always requires an expert and experienced team.
Transplantation and Temporary Bypass
Finally, ECMO sometimes plays an indispensable role as a bridge to definitive solutions, such as heart or lung transplantation. It offers the patient a chance of temporary stabilization, allowing their vital functions to be maintained until a transplant becomes available.
This temporary bypass function combines the immediate benefits of ECMO with the long-term advances brought about by transplantation, thus creating a coherent and integrated therapeutic pathway.
Conclusion
ECMO truly stands out from other life-support solutions. By combining respiratory and cardiac support while minimizing mechanical ventilation-induced injury, it constitutes a valuable therapeutic option. However, its implementation requires high-level expertise as well as appropriate technical resources, thus highlighting the importance of a careful assessment of each patient's context before making a decision.
The Future of ECMO and Innovations
Current Research and Future Developments
ECMO continues to evolve thanks to major scientific and technological advances, aimed at improving clinical outcomes while expanding its applications. Current research is focused on several priority areas, including optimizing care protocols, improving the materials used, particularly for oxygenators, and reducing the complications commonly associated with ECMO. One of the most promising areas concerns the development of more portable and easier-to-use ECMO systems. By offering greater patient mobility, these systems could revolutionize patient care, making it easier to integrate these devices into more dynamic and community-based care. For example, solutions like Cardiohelp® are already being used to support certain patients during critical periods, such as while awaiting transplantation or functional recovery. Clinical validation of their efficacy is underway and could pave the way for even wider use in various therapeutic contexts. In parallel, research efforts are focused on better selecting patient profiles eligible for this device and refining the ECMO initiation criteria. This work aims to maximize efficacy and limit risks by using more personalized and targeted approaches. Implementing strategies tailored to each patient's specific needs would ensure optimal results while reducing adverse effects. ECMO as a bridge to recovery or transplantation: ECMO now plays a crucial role in the management of patients awaiting recovery or transplantation. Its role is to provide vital support while allowing patients to remain clinically stable and sometimes even active, an important aspect in cases such as multiple organ transplants or life-threatening conditions. In the context of multi-organ thoracic transplants, ECMO has demonstrated its value by increasing short-term survival rates, although long-term data still require further investigation. In specific contexts, particularly heart-lung, heart-kidney, or lung-kidney transplants, patients on ECMO exhibit survival rates comparable to those of non-bridged patients after the critical 30-day post-transplantation milestone. Once this initial phase is over, clinical results tend to align, confirming the strategic importance of ECMO in this specific context. In lung transplantation, ECMO offers an innovative approach often referred to as a "bridge to candidacy." This strategy allows patients to benefit from continuous physical activity and remain integrated into active therapeutic protocols, thus improving their chances of success following the procedure. This approach is particularly relevant for patients suffering from acute exacerbations related to chronic lung diseases, opening new perspectives for profiles that would previously have been considered ineligible for transplantation. Regarding heart transplantation, ECMO also plays an important role, especially in complex postoperative situations, such as the onset of acute graft failure (AGF). In these specific cases, veno-arterial ECMO (VA-ECMO) provides both circulatory and respiratory support, thus offering the transplanted heart a precious chance of recovery. This intervention not only helps reduce mortality related to EGF, but also helps control postoperative complications, significantly improving the overall prognosis for the patients concerned.
Conclusion
Extracorporeal membrane oxygenation (ECMO) is now positioned as an essential life support technique for patients in acute respiratory or cardiac distress. Thanks to its ability to simulate heart and lung function, ECMO has proven highly effective in managing critical situations such as acute respiratory distress syndrome (ARDS), severe cardiogenic shock, and even major health crises like the COVID-19 pandemic. To optimize clinical outcomes, it is essential to have a thorough understanding of the eligibility criteria, monitoring parameters, and ethical considerations associated with this technique. These elements are the cornerstones for using ECMO appropriately and safely. Advances in medical research continue to refine treatment protocols, improve oxygenator materials, and perfect monitoring strategies. All of this underscores the importance of training and collaboration among medical teams. ECMO can thus act as a bridge to recovery or even transplantation, opening an invaluable avenue of hope for critically ill patients. In summary, ECMO represents a powerful tool against acute cardiorespiratory failure. It is essential to encourage further research, standardize protocols, and strengthen the skills of medical personnel. This methodical approach will maximize the benefits of this technology. By integrating ECMO judiciously and in a planned manner into intensive care, we can aspire to improved survival rates and a better quality of life for critically ill patients.
FAQ
What are the main indicators for the use of ECMO in cases of severe heart or respiratory failure?
The use of ECMO (Extracorporeal Membrane Oxygenation) in situations of severe heart or respiratory failure is based on several specific indicators:
- Acute respiratory failure: a P/F ratio (partial pressure of oxygen in the blood relative to the fraction of inspired oxygen) less than 80 mmHg with FiO2 = 1 for at least 3 hours, or less at 50 mmHg with FiO2 = 1 despite optimization of ventilatory parameters.
- Heart failure: persistence of shock despite maximal treatment, illustrated by criteria such as systolic blood pressure < 100 mmHg, high doses of dobutamine (> 10 μg/kg/min) or adrenaline (> 0.5 μg/kg/min), as well as other signs such as oliguria, mean pulmonary arterial pressure > 25 mmHg or multi-organ failure.
How does ECMO differ from conventional life support techniques, and what are its specific advantages?
Unlike conventional techniques, ECMO allows for the temporary bypassing of the heart and lungs. This maintains blood circulation and blood gas balance (oxygen and carbon dioxide) without requiring direct treatment of cardiac or pulmonary pathologies. Among its specific advantages, we can note:
- The ability to offer respite to organs by allowing them to recover after serious events such as severe acute respiratory illness, myocardial infarction, or major trauma.
- Its essential role in supporting patients who do not respond to traditional treatments in cases of severe heart or respiratory failure.
What are the potential risks and complications associated with ECMO, and how are they managed?
ECMO is not without risks. Several complications can occur, including:
- Bleeding, sometimes severe, particularly in the brain.
- Catheter-related infections.
- Blood clots or air bubbles in the tubing.
- Limb ischemia related to cannula placement.
These complications are managed by using anticoagulants to prevent thrombosis, sterile techniques to reduce infection, and reperfusion catheters to limit ischemia. Close monitoring, including echocardiograms and chest X-rays, allows for the rapid detection and treatment of other complications such as left ventricular distension or pulmonary edema.
When can ECMO serve as a "bridge" for patients awaiting a heart or lung transplant, and what are the criteria for its use?
ECMO can prove invaluable as a "bridge" for patients awaiting transplantation in critical situations:
- Bridge to lung transplantation: It optimizes respiratory and hemodynamic functions, thus facilitating the wait for a graft and potentially replacing conventional extracorporeal circulation during transplantation. It is also used in cases of primary graft failure.
- Bridge to heart transplantation: ECMO, particularly in veno-arterial form (VA-ECMO), helps patients with severe heart failure by ensuring effective organ perfusion. It also allows the transplanted heart to "rest" after transplantation with primary graft dysfunction (PGD).
Criteria include significant hemodynamic instability, acute failure of cardiac or respiratory functions, and the inability to wean from cardiopulmonary bypass after cardiac surgery. Patients are assessed based on several factors, including their functional status, their waiting time on the transplant list, and their need for mechanical ventilation.




