Criterion 2.3-10: Controlling major obstetric risks for maternal and fetal safety
What is Criterion 2.3-10?
Criterion 2.3-10, as defined in the sources, concerns the implementation by healthcare teams of measures to prevent major obstetric risks. This is a fundamental issue in the care of pregnant women and requires teams to be trained to quickly detect potential complications.
Why is Criterion 2.3-10 essential?
Preventing major obstetric risks is a central issue to guarantee the safety of patients and their newborns. This criterion is crucial because it aims to anticipate and limit the consequences of serious complications such as postpartum hemorrhage (PPH), preeclampsia, or dystocic deliveries. PPH, for example, is one of the top three causes of maternal death in France, defined as blood loss exceeding 500 mL during delivery or in the 24 hours following. Complications related to postpartum hemorrhage (PPH) can be severe, including hemorrhagic shock, complications related to transfusions or invasive surgical treatments, as well as long-term psychological sequelae.
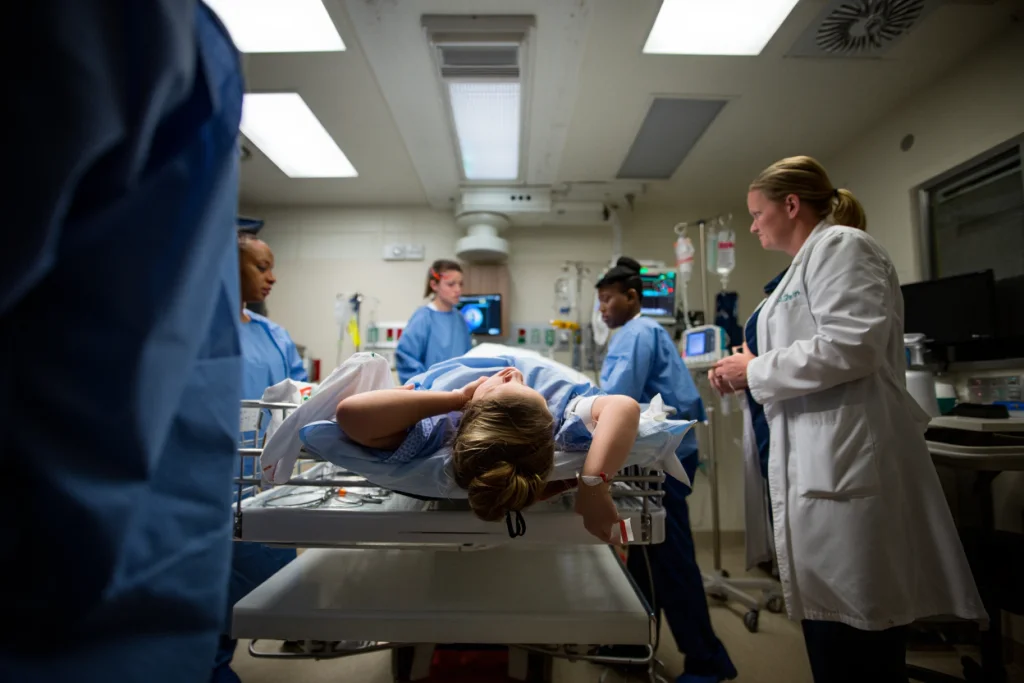
How does the Criterion Is 2.3-10 being implemented?
The implementation of Criterion 2.3-10 relies on several organizational and technical pillars:
- Rapid detection and strict protocols: Teams apply protocols to anticipate risks, with enhanced prenatal monitoring for at-risk patients and effective management of obstetric emergencies.
- Emergency simulation and fluid communication: The implementation of emergency simulations and effective communication between the various stakeholders are essential to ensure optimal responsiveness.
- Mastery of professional skills: Teams must master the interpretation of fetal heart rate (FHR) and obstetric maneuvers through specific training.
- Protocol Testing and Evaluation: The patient pathway must be tested by the team through simulation, and indicators are monitored to assess compliance with the color-coded indications and timeframes.
Safeteam Training: P24 and P34 in Support of Criterion 2.3-10
Safeteam's P24 and P34 training courses are directly aligned with the objectives of Criterion 2.3-10 by focusing on risk management, teamwork, and skills development for professionals.
P24 Training: Optimizing Cesarean Section Management Code Red
The P24 training course "Optimizing the Management of Code Red Cesarean Sections" (P24) is designed for professionals who perform emergency cesarean sections. It aims to master the key stages of care and to structure and secure teamwork when performing an absolute emergency cesarean section.
- Code Red represents an immediate life-threatening risk to the mother or child, requiring an emergency cesarean section with a decision-to-extraction time of less than 15 minutes. Code Red indications include fetal bradycardia (without recovery of the fetal heart rate within 10 minutes), failed instrumental delivery with abnormal fetal heart rate (AFHR), suspected placental abruption or retroplacental hematoma, placenta previa with severe maternal hemorrhage, suspected uterine rupture, and umbilical cord prolapse. It is important to note that maternal cardiac arrest is not classified as a Code Red, but as an extreme emergency requiring immediate fetal extraction within 5 minutes to improve maternal prognosis, without preparation or anesthesia, performed on site. The P24 training specifically covers how to react in the event of maternal cardiac arrest.
- The training uses immersive video simulation to retrace the multidisciplinary management of a patient, from the activation of code red to the performance of the cesarean section, followed by a video debriefing by field experts.
P34 Training: Management of Postpartum Hemorrhage
The P34 "Postpartum Hemorrhage" (P34) training is intended for all healthcare personnel likely to manage PPH. Postpartum hemorrhage (PPH) is a major obstetric emergency requiring a multidisciplinary team approach. The objectives of P34 training include the ability to recognize the warning signs of PPH, identify initial management actions, and understand each member's role within the team. Sources identify factors that worsen PPH, such as primiparity, a history of PPH or cesarean section, induction of labor, prolonged labor, episiotomy, general anesthesia, and multiple pregnancy. Knowledge of these factors is crucial for resource planning.
In summary, this training enables healthcare professionals to acquire and strengthen the essential technical and organizational skills to meet the requirements of Criterion 2.3-10, thus ensuring optimal and safe management of obstetric emergencies.




